

The Total Knee Replacement Case
We represented a 65- year-old man who had longstanding osteoarthritis, causing him significant knee pain while moving. He went to see an orthopaedic surgeon who recommended total knee replacement. His cartilage had worn away and he was experiencing bone on bone.
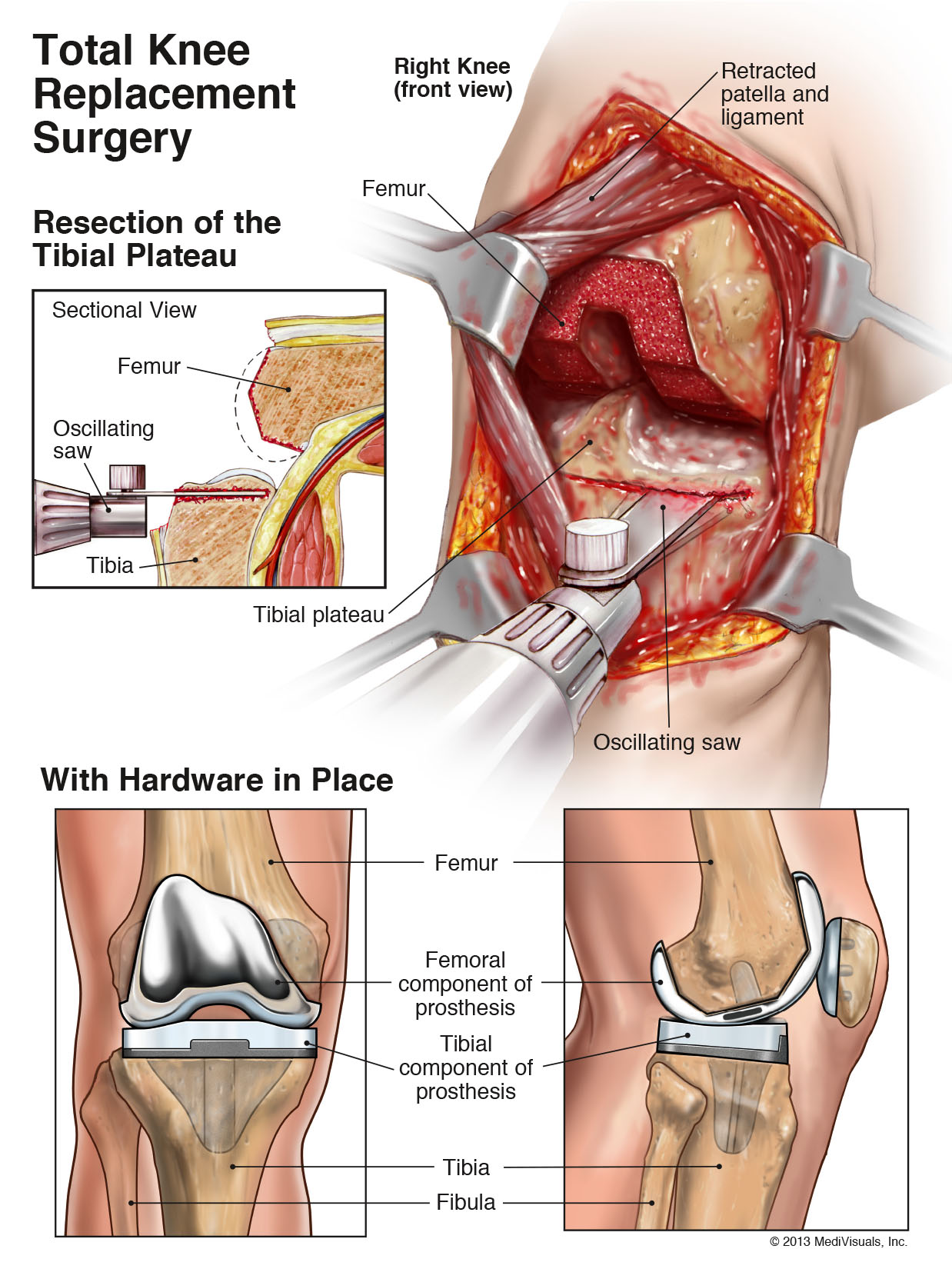
Total knee replacement involves making a large incision in the knee joint, moving the patella or knee cap over to the side, sawing off the end of the femur or thigh bone, sawing off the end of the tibia or leg bone, and replacing the knee with metal implants. A plastic spacer is inserted between the implants to achieve a relatively frictionless joint.
Knee replacement surgery is the gold standard when more conservative treatments fail, and can bring lasting relief to a pain-riddled patient.
In undertaking the orthopaedic implants, the surgeon made a standard median parapetellar incision, which would be the typical approach in placing implants in a “virgin knee,” or one which had not been previously operated on. The implants incision, at the closest point, was 1.5 cm from the old pre existing incision (see photograph at right).
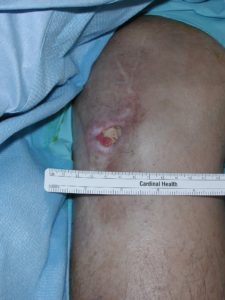 According to the leading medical text on total knee replacement, “The Techniques of Total Knee Surgery,” by Dr. Ken Krackow (1990):
According to the leading medical text on total knee replacement, “The Techniques of Total Knee Surgery,” by Dr. Ken Krackow (1990):
The greatest danger arises with placement of essentially parallel incisions and the creation of areas of ‘isolated’ skin. This kind of occurrence is potentiated by previous relatively long incisions.
The Krackow text provided a diagram showing a knee with a previous medial incision and noting that the placement of a typical medial parapetellar incision would be “unsafe” (see figure).
A narrow “skin bridge” suffers from poor blood flow (ischemia) which may lead to skin death (necrosis). The safety rule is to maintain at least 7 cm between incisions.
Within 20 days of surgery, the isolated skin between the two incisions broke down and a wound formed. The wound got infected with the bacterium pseudomonas aeruginosa. Infection over an implant is dangerous. The infection made its way deep into the knee and contaminated the implant and got into the bone.
Infection in the bone is called osteomyelitis. At that point, the care requires a two stage revision. That is, the implanted joint must be removed and an antibiotic spacer is implanted. The patient is put on IV antibiotics for six weeks. Thereafter, if possible, a new knee implant is installed.
 The patient underwent a two stage revision. However, the osteomyelitis remained. The patient got re-infected and required removal of the second knee and installation of a third knee joint. Today, the patient is at a lifetime risk for re-activation of the osteomyelitis. If and when that happens, amputation of the limb would be the most viable option.
The patient underwent a two stage revision. However, the osteomyelitis remained. The patient got re-infected and required removal of the second knee and installation of a third knee joint. Today, the patient is at a lifetime risk for re-activation of the osteomyelitis. If and when that happens, amputation of the limb would be the most viable option.
At trial, Kassel McVey Law Firm presented evidence of medical malpractice from expert witnesses that the surgeon violated the standard of care – conduct required of a reasonable and prudent surgeon under the same or similar circumstances. The experts opined that the surgeon should have incorporated or used the old pre- existing incision in placing the knee joint. Doing so would have eliminated the narrow skin bridge which broke down and led to the catastrophic results.
The defense presented as one of their experts, Dr. Krackow, the author of the text on knee replacement. Dr. Krackow tried to distinguish the patient’s knee from the one in his diagram. Ultimately, he was unsuccessful. The jury returned a verdict for the patient in the amount of $1,954,239.00.
Personal Injury Lawyers 1330 Laurel Street Columbia, SC 29201 Phone: 803-256-4242
Mailing Address
Post Office Box 1476
Columbia, South Carolina 29202
Fax: (803) 256-1952
Copyright © 2023 John D. Kassel, Attorney at Law, LLC. All rights reserved. Privacy Policy I Terms of Service | Disclaimer
This website is designed for general information only. The information should not be construed to constitute formal legal advice or the formation of a lawyer/client relationship. The results and testimonials listed on this website are specific to the facts and legal circumstances of specific cases and should not be used to form an expectation that the same results could be obtained for other clients in similar matters. This list is not a description or characterization of the quality of the firm's representation, it is not intended to compare one attorney's work to another and is in no way a guarantee of a specific result for your case.

